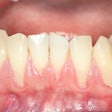
Maxwell H. Anderson, D.D.S, M.S., M.Ed., doesn't spend much time filling cavities these days. Instead, he's hard at work putting other dentists out of that business.
Dr. Anderson is CEO of C3 Jian, a California start-up that's developing medicines to suppress caries-causing bacteria. And this is just one of many companies around the country working on similar techniques that could send caries the way of polio and small pox. These new treatments would make the classic dentist's business model -- drill, fill, and bill -- as outmoded as ivory dentures.
"Within 10 years, we'll be able to eradicate caries in treatable populations," Dr. Anderson predicts. "But as a dentist, what am I left with?"
Most dentists practicing today won't have to answer that question, says Dr. Anderson. Being able to eradicate a disease isn't the same as actually eradicating it. Wiping out caries would require treating millions of Americans who don't currently have dental care. So Dr. Anderson expects the change to take place slowly.
But it has already begun and some forward-looking dentists have altered their business model as a result. Advocates of a new approach -- called caries management by risk assessment (CAMBRA) -- say dentists can make up for the lost restoration work by attracting patients with the promise of painless prevention.
The revolution has begun
If a cavity-free future sounds like fantasy, consider what has already happened in the past 30 years: the prevalence of decayed, missing, and filled permanent teeth among children aged six to 18 fell more than 60 percent, the National Health and Nutrition Examination Survey (NHANES) found. The trend for other age groups is similarly on the decline.
The likely reason: fluoridation of public water supplies and toothpaste. But most toothpaste contains fluoride and there's only so much drinking water left to fluoridate. So won't the decline in caries level off?
It might, says John Featherstone, M.Sc., Ph.D., dean of the University of California at San Francisco dentistry school, if dentists just keep handing out toothbrushes and lobbying for fluoridated water. But much more is possible.
For starters, dentists haven't exhausted the potential in fluoride. "A little fluoride is good," Dr. Featherstone said. "More fluoride is better." As a 2006 American Dental Association (ADA) panel concluded, fluoride varnishes and gels can go farther than fluoridated water and toothpaste in reducing caries. For example a Cochrane review found that patients getting varnish treatments were 46 percent less likely to need fillings than untreated patients.
And fluoride is only the beginning. Other tools in the caries preventative toolbox include:
- Antibacterials such as chlorhexidine that kill bacteria that cause caries
- Sugar-free gum with xylitol that starves bacteria while stimulating beneficial saliva flow
- Dental sealants that fill in the tooth's fissures and pits preventing decay
- Patient education to improve diet
- More frequent exams and cleanings to arrest lesions
- Applying of calcium phosphate to remineralize enamel
More techniques are in the pipeline, such as vaccines for caries bacteria and laser treatments that may render teeth more resistant to acid. Dr. Anderson's company is working on creating antimicrobial peptides (STAMPS) designed to kill only those organisms -- such as S. mutans -- that cause caries. In theory, other innocuous organisms will fill the niche left by these harmful bugs preventing a new infection.
Along similar lines, Jeffrey D. Hillman, Ph.D., D.M.D., an oral biology professor at the University of Florida, College of Dentistry in Gainesville, is trying to engineer a variety of S. mutans that doesn't produce cavity-causing acid but crowds out the virulent, naturally occurring variety.
Altogether, the prospects for stopping caries look great. But a lot of these measures can be expensive or inconvenient for patients. A 16 oz bottle of 0.12 percent chlorhexidine, for example, sells for about $100 and only lasts a couple of weeks at the recommended twice-a-day dosage.
That's where new diagnostic tools come into play. A growing body of research shows that for some people, a combination of good hygiene and ideal saliva chemistry is enough. For others, swilling chlorhexidine and getting their teeth varnished is a must. And a third group falls in the middle.
Who's next?
Common sense says dentists should concentrate their preventive efforts on those most likely to get caries. But who are they?
The simplest and most obvious way to answer that question is using guidelines based on epidemiological research. Investigators have tabulated data about age, ethnicity, class, filled surfaces, calculus, number of teeth, carious lesions, xerostomia, and a host of other factors, watching to see which ones correlate most closely with caries.
In addition, new assays can estimate the number of caries-causing bacteria in a person's saliva. And electronic devices that can catch caries in early stages are becoming cheaper and more accurate. The Diagnodent (KaVo America) uses a laser to detect the fluorescence of tooth decay. Similar, the D-Carie mini (Neks Technologies), uses light emitting diodes for the same purpose. Other new machines shine light through teeth to create images showing lesions.
With such tools literally in hand, dentists can categorize patients as high, medium, or low risk. "Caries risk assessment and subsequent [management] are what it's all about!" says Martin Davis, D.D.S., a pediatric dentist and associate dean at Columbia University. He argues that high-risk patients should be seen more than twice a year and low-risk patients perhaps every 12 to 18 months.
Since 25 percent of patients get 80 percent of fillings, combining new and old prevention techniques could mean a lot fewer cavities to fill… and a dent in your typical general dentist's wallet.