As we look ahead to 2024, it’s always interesting to predict which technologies and techniques will become a regular part of the dental industry in the near future.
Among the candidates for 2024 is third-molar tooth bud ablation, a process we covered back in 2022. During the recent American Academy of Implant Dentistry (AAID) meeting in Las Vegas, I had the chance to interview Dr. Leigh Colby about how far the science behind the technique has come since then and why dentists need to know about it and how it will impact their lives and practices.
Q&A about third-molar tooth bud ablation
1. How will ablation change dentistry in 2024?
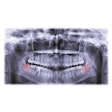
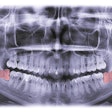
Fully guided third-molar tooth bud ablation (3TBA) will have a huge impact on how the dental profession manages third molars. Managing third molars hasn’t changed much in more than a century. We can either extract third molars early (before pathology develops) or treat patients after problems develop. Unfortunately, undoing the damage these destructive teeth cause over a patient’s lifetime is far more painful and expensive than preventive care treatment.
The controversy surrounding prophylactic removal of third molars is triggered only because of the very real trauma and serious complications that occur following third-molar removal. Fully guided 3TBA will have none of the complications associated with the surgical removal of third molars. With 3TBA, there is minimal risk of infection and no chance of painful dry socket. More important, the risk of lifelong defects -- damage to the nerves and the bony structure distal to the second molars -- will likely never occur with 3TBA.
2. What is the biggest issue that 3TBA will solve?
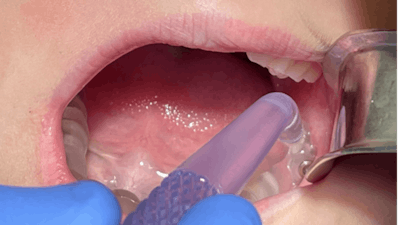
Fully guided 3TBA is designed to eliminate all the surgical trauma associated with third-molar removal. Eliminating serious side effects associated with third-molar extraction is what fully guided 3TBA is all about. 3TBA is a minimally invasive procedure that involves no more than a single puncture immediately followed by a 30-second to 90-second ablation in the center of the third-molar tooth bud. Kids should be able to immediately go out and play following 3TBA.
To make this possible, we had to solve several technical issues. Medical ablation has been used successfully to remove cancerous tumors for decades. The problem with using tumor ablation technology in dentistry is that it’s not precise enough. It’s like using a shotgun.
Medical tumor technology is designed to remove large tumors that can be 5 cm or more in diameter. In contrast, we developed and patented technology that controls the application of heat energy with a high degree of accuracy so that tissue is not charred during ablation. Our technology ensures that the center of ablation is within 0.5 mm of a tooth bud’s center. In addition, we have developed a spherical zone of ablation, which prevents damage to tissue outside of the tooth bud. Our Zero3 TBA system is the first of its kind, with soft-tissue ablation properties that no other medical ablation technology has. The technology is so precise that we can prescribe the ablation zone diameter with 0.1 mm resolution.
Our latest study, published this year by the Journal of Oral and Maxillofacial Surgery, included radiologic and histologic assessments that confirmed complete healing within 28 days of ablation treatment. There was no evidence of treatment, just bony infill within weeks following treatment. It’s just like a pediatric tooth extraction, where you expect complete bony ingrowth in a matter of weeks.
3. What is the learning curve for this technique?
Kevin, remember I trained you in less than one minute at the AAID meeting! Training takes just minutes. If you know how to place a dental implant using a surgical guide, then you already know how to perform the 3TBA procedure. Anesthesia consists of local anesthetic infiltrated on the buccal and lingual aspects of the tooth bud.
Once the 3TBA handpiece is fully seated into the custom guide, the center of ablation is positioned in the center of the tooth bud. All the operator has to do is step on a pedal to initiate the ablation process, and the ablation then occurs from the center outward. The treatment is completely controlled by our Zero3 microwave generator.
4. What do team members need to know about 3TBA?
The 3TBA procedure is faster and easier than placing an implant. The team first obtains a cone-beam computed tomography scan and dental impression, which can easily be obtained during a patent’s regular checkup. The dental office then sends the scan and impression to TriAgenics to have custom guides and microablation probes fabricated.
At the treatment appointment, local anesthesia is infiltrated on the buccal and lingual of targeted tooth buds. The bone over the tooth bud is generally spongy. If the bone is dense, a small diameter osteotomy may be necessary.
At this point, the patient is ready for treatment. Step on the generator pedal to activate an ablation cycle, and you are done in 60 seconds or less. It’s much faster (and easier) than placing a one-surface composite restoration!
5. How long do you believe it will be until this technique is commonplace in our industry?
Fully guided 3TBA represents dramatically better patient care. Oral surgeons and pediatric dentists who have been involved in this project believe fully guided 3TBA will deliver far better lifelong outcomes. Based on this, we believe 3TBA will be the industry standard of care within 10 years of introduction. The reason for this rapid change is that the 3TBA procedure is much simpler and safer than surgical removal of third molars.
Editor’s note: To learn more, visit www.TriAgenics.com or email Dr. Colby directly at [email protected].