Early treatment of poor oral health may lead to significant brain health benefits, according to preliminary research to be presented at the American Stroke Association's International Stroke Conference 2023.
A group led by Dr. Cyprien Rivier of the Yale School of Medicine in New Haven, CT, analyzed the potential link between oral health and brain health among approximately 40,000 adults without a history of stroke who were enrolled in the U.K. Biobank. They found that people who were genetically prone to cavities, missing teeth, or needing dentures had a higher burden of silent cerebrovascular disease.
"Poor oral health may cause declines in brain health, so we need to be extra careful with our oral hygiene because it has implications far beyond the mouth," Rivier said in a news release from the American Stroke Association (ASA).
According to the ASA, stroke is the No. 5 cause of death and a leading cause of disability in the U.S. Previous research has found that gum disease and other oral health concerns are linked to heart disease risk factors and other conditions like high blood pressure.
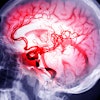
However, what isn't clear is whether poor oral health affects brain health, meaning the functional status of a person's brain, which the researchers aimed to investigate in this study using neuroimaging tools such as magnetic resonance imaging (MRI).


Signs of poor brain health in patients were detected using brain MR images of white matter hyperintensities, which may indicate impaired memory, balance, and mobility. These findings were correlated with genetic variants known to predispose individuals to cavities, dentures, and missing teeth later in life.
Between 2014 and 2021, the researchers screened participants for 105 genetic variants known to predispose individuals to cavities, dentures, and missing teeth later in life. The findings were correlated with white matter hyperintensities revealed on patients' MRI scans, which can indicate microstructural tissue damage.
The analysis found the following:
- People who were genetically prone to cavities, missing teeth, or needing dentures had a higher burden of silent cerebrovascular disease, as represented by a 24% increase in the amount of white matter hyperintensities visible on the MRI images.
- Those with overall genetically poor oral health had increased damage to the fine architecture of the brain, as represented by a 43% change in microstructural damage scores visible on the MRI scans. Microstructural damage scores are whole-brain summaries of the damage sustained by the fine architecture of each brain region.
In a comment on the research, Dr. Joseph P. Broderick of the ASA's Stroke Council said that while the study results don't demonstrate that dental hygiene improves brain health, the findings are "intriguing" and should prompt more research.
"Genetic profiles for increased risk of oral health may overlap with genetic risk factors for other chronic health conditions like diabetes, hypertension, stroke, infections that are known to be related to brain imaging markers," he said.
The American Stroke Association's International Stroke Conference, where the study will be presented, will be held in person in Dallas and virtually, February 8-10, 2023.